Stress
Learn how cortisol rhythm works, how stress disrupts it, and how nervous system regulation supports healthier stress recovery and sleep.
Cortisol is the body’s primary stress hormone, designed to follow a daily rhythm that supports energy in the morning and rest at night. Chronic stress, poor sleep, and circadian disruption can flatten or mistime this rhythm, contributing to fatigue, anxiety, metabolic issues, and sleep problems. Understanding how cortisol is regulated by the nervous system and circadian clock reveals why stress management is less about eliminating stress and more about restoring balance. Breath-based practices such as SKY Breath Meditation support nervous system regulation and may help normalize cortisol rhythms over time.
Cortisol is often referred to as the “stress hormone,” but its role in the body is far more nuanced. Rather than being inherently harmful, cortisol is essential for survival—helping regulate energy, blood pressure, immune function, and the sleep-wake cycle.
The circadian system, our internal biological clock regulated primarily by the suprachiasmatic nucleus (SCN), governs daily physiological processes and synchronizes hormone release, including cortisol, with environmental cues.
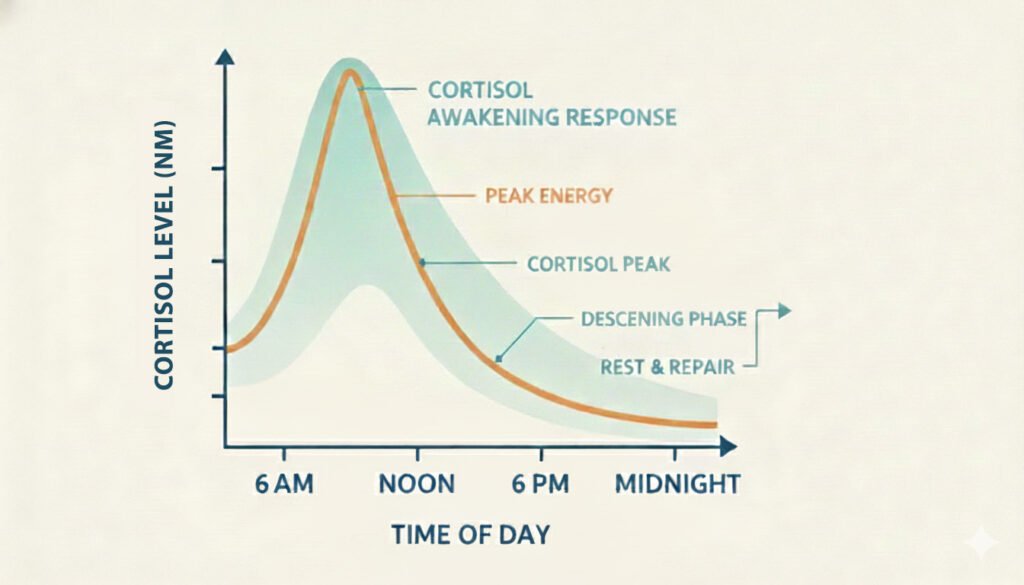
Under healthy conditions, cortisol follows a predictable daily pattern known as the cortisol rhythm, rising in the morning to support alertness and gradually declining at night to allow the body to rest and recover. Circadian rhythms are key regulators of numerous physiological processes, including hormone secretion, metabolism, immune function, and the sleep-wake cycle. When stress becomes chronic, or the nervous system remains stuck in high alert, this rhythm can become disrupted, leading to a wide range of physical and mental health symptoms.
Understanding cortisol rhythm offers a clearer lens for stress management—one that focuses on regulation rather than suppression.

Cortisol is a steroid hormone produced by the adrenal glands, which sit atop the kidneys. Cortisol is synthesized in the adrenal cortex, specifically in the zona fasciculata, which is responsible for producing this and other steroid hormones. It plays a central role in helping the body respond to stress and maintain internal balance.
Cortisol helps:
Cortisol exerts its effects by binding to glucocorticoid receptors, which are widely distributed throughout the body.
Rather than acting in isolation, cortisol operates as part of an integrated brain-body system designed to respond to both physical and psychological demands.
Cortisol production is regulated by the hypothalamic-pituitary-adrenal (HPA) axis, a communication network between the brain and endocrine system.
The process works as follows:
Feedback loops within the HPA axis help regulate cortisol levels so they rise when needed and fall during periods of rest. Chronic stress can interfere with these feedback signals, leading to cortisol dysregulation rather than healthy responsiveness.
Adrenal insufficiency can occur when the adrenal glands do not produce enough cortisol, disrupting the normal cortisol rhythm. There are two main types: primary adrenal insufficiency, often caused by autoimmune attacks that damage the adrenal glands (as seen in Addison’s disease), and secondary adrenal insufficiency, which results from pituitary gland dysfunction or abrupt cessation of corticosteroid treatment. Both conditions affect the physiological regulation of cortisol within the HPA axis and can significantly affect hormone balance and overall health.

Cortisol exhibits a diurnal rhythm closely linked to the circadian clock:
Cortisol levels are low at the beginning of sleep, rise toward the end, and peak just before waking. The cortisol awakening response (CAR) is characterized by a significant surge in cortisol levels shortly after waking, which prepares the body for daily demands.
This rhythm is coordinated by the suprachiasmatic nucleus (SCN) in the brain, which synchronizes hormonal timing with light-dark cycles. The central clock in the SCN synchronizes with peripheral clocks in tissues throughout the body to coordinate hormonal timing. Melatonin secretion is also regulated by the circadian system and interacts with cortisol rhythms. When this system is functioning well, cortisol supports both productivity and recovery.

Stress is not the problem—unresolved stress is. Acute stress temporarily elevates cortisol and then resolves. Chronic stress, however, repeatedly activates the HPA axis.
Common disruptors include:
Night-shift workers often experience a phase shift in cortisol rhythms, with peak levels occurring at inappropriate times. Circadian rhythm misalignment from night-shift work can increase the risk of developing type 2 diabetes and obesity by disrupting circadian rhythms and altering hormone secretion patterns.
Over time, cortisol rhythm may become flattened, elevated at night, or mistimed—patterns associated with fatigue, sleep disruption, emotional reactivity, and metabolic strain.
| Aspect | Healthy cortisol rhythm | Disrupted cortisol rhythm |
| Morning levels | Strong, timely morning rise | Blunted or delayed rise |
| Daytime pattern | Gradual decline throughout the day | Erratic or flattened pattern |
| Evening levels | Low by bedtime | Elevated late at night |
| Sleep impact | Easier sleep onset, deeper rest | Difficulty falling or staying asleep |
| Energy levels | Alert in the morning, steady energy | “Tired but wired” or daytime fatigue |
| Stress recovery | Efficient return to baseline after stress | Prolonged stress activation |
| Nervous system tone | Balanced sympathetic and parasympathetic activity | Sympathetic dominance |
| Long-term effects | Resilience and metabolic balance | Anxiety, burnout, metabolic strain |

When cortisol rhythm is disrupted, the effects can ripple through nearly every system in the body.
Common consequences include:
Adipose tissue plays a significant role in metabolic regulation and local cortisol activation, contributing to insulin resistance and inflammation.
Chronic dysregulation of cortisol is associated with a higher risk of cardiovascular disease, depression, and a shorter lifespan. Over time, it can also lead to long-term health issues such as type 2 diabetes, hypertension, and cognitive decline.
Rather than indicating a single hormonal problem, these symptoms often reflect nervous system dysregulation and impaired stress recovery.

Cortisol plays a pivotal role in the cardiovascular system, acting as a key regulator of blood pressure, heart rate, and vascular tone. Produced by the adrenal glands, cortisol secretion follows a circadian rhythm that helps maintain stable blood pressure and ensures that vital organs like the brain and muscles receive adequate blood flow throughout the day.
Under normal conditions, cortisol release is tightly controlled by the body’s internal clock, or circadian clock, which is governed by the suprachiasmatic nucleus (SCN) in the brain. This central clock synchronizes hormone secretion—including cortisol production—with the 24-hour light-dark cycle, supporting optimal cardiovascular function. When circadian rhythm regulation is disrupted, for example, by shift work, chronic stress, or sleep deprivation, cortisol levels may become elevated or misregulated, placing additional strain on the cardiovascular system.
Excess cortisol, especially when driven by chronic stress or HPA axis dysfunction, can have significant consequences for cardiovascular health. Persistently high cortisol levels contribute to increased blood pressure, vascular stiffness, and even cardiac hypertrophy. Over time, these changes raise the risk of developing cardiovascular disease, including myocardial infarction and stroke. Cortisol also influences glucose and lipid metabolism, both of which are closely linked to cardiovascular risk factors such as insulin resistance and metabolic syndrome.
The relationship between cortisol and the cardiovascular system is further complicated by its effects on the immune system and sleep quality. Poor sleep or sleep disturbances can disrupt cortisol secretion, leading to elevated nighttime cortisol and further increasing cardiovascular morbidity. Conversely, healthy sleep supports circadian regulation of hormone secretion, helping to protect the heart and blood vessels.
The hypothalamic-pituitary-adrenal (HPA) axis is central to this process. When the pituitary adrenal HPA axis is dysregulated—whether due to chronic psychological stress, circadian misalignment, or other factors—cortisol production can become excessive or insufficient, both of which negatively impact cardiovascular health.
In summary, cortisol contributes to the cardiovascular system’s delicate balance, and its rhythmic secretion is essential for maintaining cardiovascular health. Disruptions in cortisol rhythm—whether from chronic stress, poor sleep, or circadian disruption—can increase cardiovascular risk. By supporting healthy cortisol levels and circadian rhythm regulation through lifestyle practices and stress management, it’s possible to reduce cardiovascular morbidity and promote long-term well-being.
Cortisol output is closely tied to autonomic nervous system tone. When the sympathetic nervous system (fight-or-flight) dominates, the HPA axis receives frequent signals to stay activated.
Healthy cortisol rhythms depend on the body’s ability to shift into parasympathetic (rest-and-digest) states. This shift signals to the brain that it is safe to reduce stress signaling and allow cortisol to decline at appropriate times.
This is why stress-management approaches that directly support nervous-system regulation are particularly effective.

SKY Breath Meditation is a structured breathing practice that works with the breath–nervous system connection to support physiological balance.
Research on breath-based practices suggests they may:
Rather than forcing cortisol levels down, SKY Breath Meditation helps create the internal conditions that allow cortisol rhythms to normalize naturally. Over time, this can support:
This approach aligns with modern stress science, which emphasizes regulation over suppression.
Cortisol balance is shaped by daily habits that act as timing cues for the nervous system.
Supportive practices include:
Small, consistent routines help retrain the body’s internal clock.
Cortisol testing may be useful when symptoms persist or remain unexplained. Common methods include:
Results are most meaningful when interpreted alongside sleep quality, stress load, and nervous system symptoms rather than viewed in isolation.
Stress is unavoidable. What determines health outcomes is how efficiently the body recovers.
A well-regulated cortisol rhythm reflects a nervous system that can respond to challenge and return to balance. Practices that support regulation—sleep, breath, movement, and social connection—are more sustainable than attempts to eliminate stress altogether.

Cortisol is not the enemy; dysregulation is. A healthy cortisol rhythm supports energy, focus, and recovery, while chronic disruption undermines both physical and mental well-being.
Understanding how stress, circadian rhythms, and the nervous system interact clarifies why breath-based practices such as SKY Breath Meditation are effective tools for long-term stress resilience. Restoring balance is less about control and more about creating the conditions for the body to self-regulate.
Understanding the Science of Mental Hyperarousal: Causes and Solutions for Sleep and Anxiety
The cortisol rhythm is the body’s natural daily pattern of cortisol release. Cortisol levels typically peak in the early morning to support alertness and gradually decline throughout the day, reaching their lowest point at night to support sleep and recovery.
Acute stress temporarily elevates cortisol to facilitate the body’s response. Chronic stress can disrupt cortisol circadian timing, leading to elevated evening cortisol, flattened daily rhythms, or impaired stress recovery.
Yes. Persistently high or mistimed cortisol is associated with anxiety, sleep disruption, and metabolic issues, while low or poorly responsive cortisol may contribute to fatigue and low stress tolerance. Both often reflect nervous system dysregulation rather than a single hormone problem.
The hypothalamic-pituitary-adrenal (HPA) axis is the system that regulates cortisol production. It connects the brain and adrenal glands to coordinate the stress response and maintain hormonal balance.
Cortisol and sleep are closely linked. Healthy cortisol levels rise in the morning and fall at night. Elevated evening cortisol can make it difficult to fall or stay asleep, while poor sleep can further disrupt cortisol rhythm.
Breathing practices that support nervous system regulation may help normalize cortisol rhythms over time by reducing excessive stress signaling and improving parasympathetic activity.
SKY Breath Meditation uses structured breathing patterns to support autonomic balance. By calming the nervous system, SKY may help restore healthier cortisol timing and improve resilience to daily stress.
Cortisol testing may be helpful in some cases, particularly when symptoms persist. Results are most meaningful when interpreted in the context of sleep patterns, stress levels, and lifestyle factors.












